Atopic Dermatitis and Gut Health: Healing the Skin by First Healing the Gut
Atopic Dermatitis and Gut Health: Healing the Skin by First Healing the Gut
Many people come to my clinic and say the same thing:
“We apply steroid cream every day, but it doesn’t really get better…”
“My child scratches all night, and we’re both exhausted…”
When treatment isn’t working, most people assume the problem is still on the skin. But atopic dermatitis is not just a skin disease. It is a whole-body inflammatory condition, deeply connected to the gut. Unless we address what’s happening inside, medications alone can’t bring true improvement.
Why Medication Alone Doesn’t Lead to Real Healing
The skin only shows the “result” of what’s happening in the body. If the intestinal barrier is weak or inflamed, the skin continues to react no matter how much cream we apply. One mother told me: “Doctor, my child slept through the night for the first time!” This was only a few weeks after we started supporting his gut environment—not after changing his skin medication.
The Growing Reality of Atopic Dermatitis
Atopic dermatitis often comes with:
- intense itching
- redness and swelling
- very dry skin
- increased infections from scratching
- Many children also develop allergies, asthma, or hay fever.
This happens because a weakened skin barrier allows allergens to enter more easily.
The numbers speak for themselves:
1980s: 1 in 30 schoolchildren had atopic dermatitis
Today: 1 in 10
Children under age 3: 13.2% and increasing
Something inside the body—not just the skin—is driving this rise.
How the Gut and Skin Are Connected
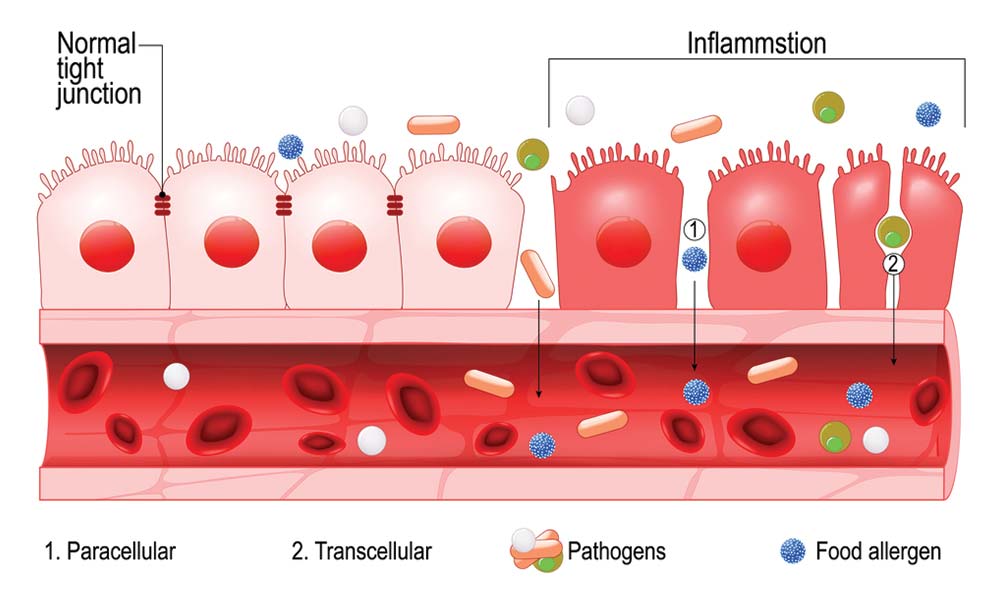
- The Intestinal Barrier: The Body’s “Front Door”
The intestinal lining works like a smart filter—absorbing what the body needs while blocking harmful substances. But when “leaky gut” develops, tiny gaps open in that barrier. Undigested food particles, toxins from bacteria, and irritants pass into the bloodstream and trigger inflammation everywhere—including the skin. If this barrier remains open, the skin continues to flare.
- Imbalanced Gut Bacteria Worsen Skin Symptoms
A healthy gut has the right balance of beneficial and harmful bacteria. When this balance collapses:
- allergic reactions worsen
- inflammatory bacteria increase
- the intestinal lining becomes weaker
- the immune system stays overstimulated
In fact, people with atopic dermatitis often show clear differences in their gut microbiome compared to healthy individuals.
- Mucin: The Invisible Shield Protecting the Gut
Mucin is a gel-like mucus that covers and protects the intestines. If the intestinal lining is the “front door,” mucin is the lock and chain that keeps it secure. Even a strong door is unsafe without a lock.
Bacteria That Break Down Mucin
Certain harmful bacteria weaken this protective layer:
- Ruminococcus gnavus and toxin-producing Bacteroides Prevotella (thrives when diets are high in fat or sugar)
- Desulfovibrio (produces hydrogen sulfide that damages the intestinal lining)
I once treated a woman in her 30s whose atopic symptoms worsened every time work stress led to a poor diet. Once we focused on rebuilding her gut, she told me:
“My skin feels calmer… and my makeup goes on so much smoother.”
Everyday Habits That Damage the Mucin Layer
Dietary habits
- Too much greasy or sugary food
→ Increases harmful bacteria and weakens the gut barrier.

- Not enough dietary fiber
→ When gut bacteria lack food, they “eat” the mucin layer instead.
- Excessive meat, especially processed meat
→ Raises sulfur compounds that feed bacteria producing harmful gases.
- Frequent alcohol
→ Makes the intestinal lining more permeable and disrupts the microbiome.
Lifestyle habits
- Chronic stress and insufficient sleep
→ Reduce the body’s ability to produce protective mucus.
- Overuse of antibiotics or pain relievers
→ Kills beneficial bacteria and damages the intestinal lining.
How to Support Mucin and Protect the Gut
Here are practical steps I often share with patients:
- Fermentable dietary fiber
Foods like:
- oatmeal
- onions
- burdock root
- bananas
- seaweed

These increase short-chain fatty acids such as butyrate, which stimulate mucin
production.
- Resistant starch
Found in:
- cooled rice or pasta
- unripe bananas
- beans
This helps beneficial bacteria grow and thickens the mucus layer.
- Polyphenols
Rich in:
- green tea
- turmeric
- pomegranates
- blueberries
- cacao
Polyphenols reduce inflammation and protect the intestinal barrier.
- Key nutrients for mucosal repair
- Glutamine — repairs intestinal cells
- N-acetylglucosamine — a building block of mucin
- Akkermansia-friendly probiotics — support the mucin layer
My Family’s Experience
My eldest son developed atopic dermatitis at just three months old. We noticed his symptoms improved whenever my wife avoided certain foods while breastfeeding. As he grew, we supported his gut with polyphenol-rich fruits like blueberries and blackberries. His symptoms gradually became milder. Even now, when he eats junk food or snack foods with additives, his skin quickly becomes rough. Through experience, he learned the connection between diet and his skin—and became careful on his own
The Essential First Step to Improving Atopic Dermatitis
To truly improve atopic dermatitis, we must start inside the body, not on the surface. Skin medications are helpful—they soothe symptoms. But healing the intestinal barrier removes the source of inflammation.
Practical steps:
- Reduce foods and habits that weaken the mucin layer
- Eat fermentable fibers and resistant starch regularly
- Add polyphenol-rich foods to calm inflammation
- Support the intestinal lining with key nutrients
When the gut becomes stronger, the skin finally has a chance to heal.
References
-
1 Lee, S. Y., et al. (2018). Microbiome in the gut-skin axis in atopic dermatitis. Allergy, Asthma & Immunology Research, 10(4), 354–362. Comprehensive review of the gut-skin axis. Provides the foundational concept for the entire article.
-
2 Desai, M. S., et al. (2016). A dietary fiber-deprived gut microbiota degrades the colonic mucus barrier and enhances pathogen susceptibility. Cell, 167(5), 1339–1353.e21. Supports the article's core claim that dietary fiber deficiency disrupts the mucus layer.
-
3 Johansson, M. E., et al. (2014). The inner of the two Muc2 mucin-dependent mucus layers in colon is devoid of bacteria. Science Translational Medicine, 6(253), 253ra123. Fundamental literature explaining the barrier function of the mucin layer. Mucin-degrading bacteria
-
4 Crost, E. H., et al. (2013). Utilisation of mucin glycans by the human gut symbiont Ruminococcus gnavus is subject to complex genetic regulation. PNAS, 110(27), 10940–10945. Demonstrates R. gnavus's mucin-degrading capability.
-
5 Ijssennagger, N., et al. (2016). Sulfide as a mucus barrier-breaker in inflammatory bowel disease? Trends in Molecular Medicine, 22(3), 190–199. Mechanism of Desulfovibrio genus hydrogen sulfide production breaking down the barrier. Beneficial Gut Bacteria
-
6 Zhang, T., et al. (2019). Akkermansia muciniphila is a promising probiotic. Microbial Biotechnology, 12(6), 1109–1125. Comprehensive review of the beneficial effects of A. muciniphila. Short-chain fatty acids
-
7 Furusawa, Y., et al. (2013). Commensal microbe-derived butyrate induces the differentiation of colonic regulatory T cells. Nature, 504(7480), 446–450. Important study demonstrating the immunomodulatory effects of butyrate. Stress and the Intestinal Barrier
-
8 Wang, Y., et al. (2021). Stress-induced disruption of intestinal barrier and mucosal immunity. Frontiers in Immunology, 12, 631840. Latest review on the mechanism by which stress disrupts the intestinal barrier. N-Acetyl Glucosamine
-
9 Dharmani, P., et al. (2009). Role of N-acetyl glucosamine in colonic mucosal protection and repair. Inflammatory Bowel Diseases, 15(7), 1073–1083. N- acetyl glucosamine's mucin production-promoting effect. Clinical Research on Gut Bacteria and Atopic Disease
-
10 Nylund, L., et al. (2015). Severity of atopic disease inversely correlates with intestinal microbiota diversity and butyrate-producing bacteria. Allergy, 70(2), 241–244. Demonstrated inverse correlation between atopic disease severity and gut microbiota diversity.
-
* These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease.

 US Dollar
US Dollar

